Connecting state and local government leaders
New data shows that current treatment, testing and prevention methods are not reaching enough Americans to help curtail new HIV cases, which federal officials said underscores the need for expanded options.
HIV testing, treatment and preventive measures are not reaching enough Americans, leading to stalled progress in lowering the transmission of the virus, federal officials said Tuesday.
The data, released this week in a report by the Centers for Disease Control and Prevention, comes after the Trump administration announced that it wants to reduce new infections by 90 percent in the United States within the next decade. The report highlights the steps necessary to pursue that goal, including the need for increased outreach, particularly in communities that account for disproportionate numbers of new diagnoses, said Dr. Eugene McCray, director of the Center for Disease Control and Prevention’s Division of HIV/AIDS Prevention.
“These findings underscore the urgent need to rapidly scale up HIV treatment, testing and (preventive medication),” McCray said Tuesday on a media call. “We know our national goals can be achieved.”
According to the report, 14 percent of people with HIV (about 154,000) in 2017 were unaware of their status, and only 63 percent of people who knew they had HIV were treating the virus appropriately.
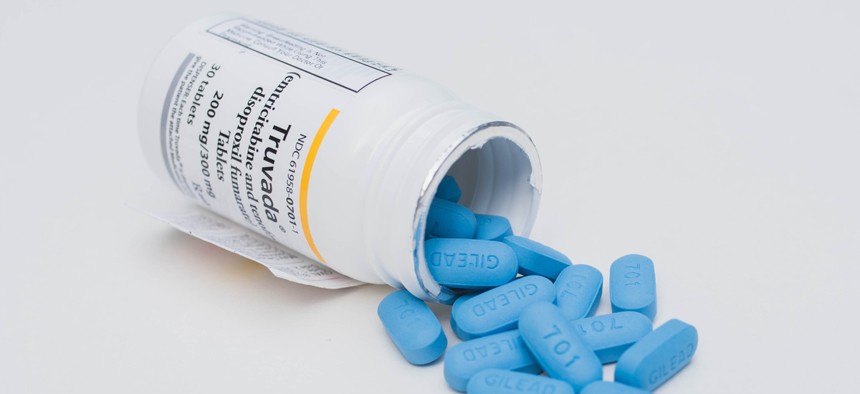
Populations at risk of getting HIV (gay and bisexual men, young people, African Americans and Latinos) could benefit from pre-exposure prophylaxis, or PrEP, a daily pill marketed as Truvada that helps prevent transmission—but only 18 percent of people deemed at risk had received a prescription for the medication as of last year. Those factors contributed to a “stalling” in the decline of new diagnoses, which have held steady at about 38,000 per year since 2013.
“In this case,” McCray said, “stability is not good.”
A proposed federal initiative would aim to reverse that trend by addressing disparities in HIV testing, treatment and prevention. Immediate steps include giving free doses of PrEP to people at risk of contracting HIV who have tested negative for the virus and have valid prescriptions, but do not have prescription drug coverage.
Federal officials have also identified 57 geographic areas (including 48 counties, Washington D.C. and San Juan, Puerto Rico) that account for more than 50 percent of new HIV diagnoses. Officials in those areas are currently working on local solutions, according to Dr. Jay C. Butler, the CDC’s deputy director of infectious diseases.
“We recognize that there need to be different actions taken in different communities” he said. “In each jurisdiction, they are developing individual plans to unstop that stalling in the decline of new cases.”
The full initiative hasn’t been funded, though the federal Department of Health and Human Services has provided money to three communities—Baltimore, Maryland.; DeKalb County, Georgia and East Baton Rouge Parish, Louisiana—to “jumpstart” the process and report back about what works and what doesn't. Broadly, the priority areas are defined as diagnosing people as early as possible, treating them effectively, preventing new transmissions and responding quickly to potential outbreaks.
“This is an ambitious goal,” Butler said. “But with swift and bold action, not only is it achievable, we can get it done.”
Kate Elizabeth Queram is a Staff Correspondent for Route Fifty and is based in Washington, D.C.

NEXT STORY: A Town Moves Forward After Two 'Thousand-Year' Storms