Connecting state and local government leaders
“We get quarterly, sometimes monthly economic data, but when it comes to drug overdoses we have to wait two years. It’s about setting priorities. It’s absolutely insane.”
Editor’s Note: On Sunday afternoon, U.S. county government leaders packed a ballroom at the Marriott Wardman Park hotel in Washington, D.C., for a National Association of Counties town hall meeting on the opioid abuse epidemic, a public health crisis ravaging many communities across the nation and a top priority for NACo and other government associations.
Featured panelists included Boone County, Kentucky, Judge Gary Moore, the co-chair of the national city-county opioid task force, Kentucky; Loudoun County, Virginia, Board Chair Phyllis Randall, a mental health therapist; and Stephen Williams, the mayor of Huntington, West Virginia, whose city has become a poster child for the epidemic. In a recent special report on health data, Route Fifty profiled Huntington’s struggles to respond to the opioid crisis, including the challenges to get timely data that can help improve response from local agencies.
Below, we’re rerunning Staff Correspondent Quinn Libson’s in-depth feature on Huntington and the opioid crisis. To download the health data special report in full, click here. For Route Fifty’s complete coverage of the opioid crisis, click here.

June 3, 2011, is a date that is stuck in Scott Lemley’s head.
Lemley is the criminal intelligence analyst for the police department in Huntington, West Virginia, and, as he sees it on that particular summer day, nearly six years ago and roughly 750 miles away, something happened that set a course that would change his job, and lead to tragic consequences for life in Huntington and elsewhere around the nation.
That June, the state of Florida—the point of origin of the majority of West Virginia’s illicit opioid painkiller prescriptions at the time—began to crack down on its notorious pill mills. On that day, Florida Gov. Rick Scott signed H.B. 7095 into law, a bill that threatened disciplinary action against doctors who unscrupulously prescribed painkillers, attached additional regulations to the prescribing of these controlled substances and strengthened state power over pill trafficking.
By all accounts, this bill did what it was intended to do. In 2010, the U.S. Drug Enforcement Administration reported that 90 of the country’s top 100 oxycodone purchasing doctors were located in Florida. Just three years later, in a 2013 press release, the DEA proudly wrote that not a single Florida doctor made it onto that same list.
But, as is known now, that remarkable success had unintended consequences.
Looking back at the data, Lemley says “you can just watch it from 2011 onwards. It’s literally a switch that happened.”
The “switch” Lemley is referring to has been well-documented. As Florida’s pill mills shut down, the prescription drugs that did make it from the Sunshine State to places like Huntington tripled in street value. The people who were addicted to those pills didn’t recover from their opioid dependency. They switched to something cheaper and easier to attain—heroin.
In the six years since June 3, 2011, Huntington has become the poster child of the nationwide opioid epidemic.
In August 2016, the city made national headlines when 26 people overdosed within the span of hours. All 26 survived, but too many in Huntington aren’t so lucky.
The city sees the most opioid overdose deaths in the entire state of West Virginia, a state that leads the nation in that same statistic.
“We didn’t see that coming. I should have, a lot of us should have. But we didn’t,” says Lemley.
‘Oh My God, It’s in My Neighborhood Too’
For the past three years it has been Scott Lemley’s job to examine all the available data and spot tragic new trends—like the surge in heroin use—coming before they hit.
Lemley has been monitoring crime data for the Huntington Police Department for the last six and a half years. As part of that job he tracks everything from car break-ins to issues of homeland security.
Three years ago, acknowledging the wicked problem of opioid addiction in Huntington, Mayor Stephen Williams created the Mayor’s Office of Drug Control Policy to carry out a multi-layered approach to the city’s heroin crisis. Now, Lemley spends about 50 percent of his time gathering and analyzing data directly related to every facet of opioid abuse.
At first Lemley focused his analysis on crime data—where drug offenses occur, what time of day, where they occur, what types of drugs are found, ect. Some of the first products of that work blew him away.
Using heat-mapping, Lemley created two maps. The first showed the location of drug offenses within the city of Huntington in 2004. At that point, the majority of those drug offenses involved crack and cocaine, and they were located in predominantly African-American neighborhoods.
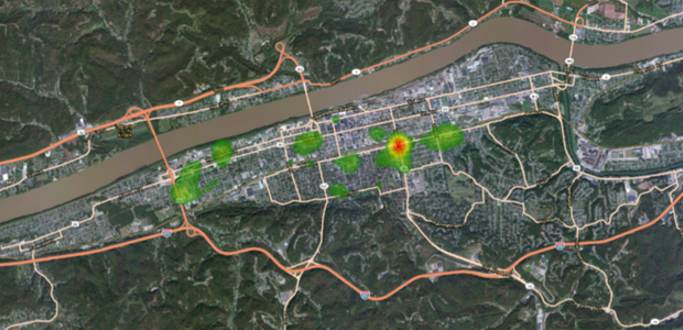
At that time, Lemley said, “you could narrow [the drug crime] down to a two block by four block radius.”
Then, he put together the heat map for 2014. The difference is clear even to a completely untrained eye. “There is no neighborhood where drug crime does not touch now,” Lemley said. And now, the majority of those crimes involve heroin.
It’s the kind of map that draws gasps when Lemley shows it. In Huntington, heroin has no age group, it’s not based on sex or income or education or location. As Lemley point out, “it’s everywhere.”
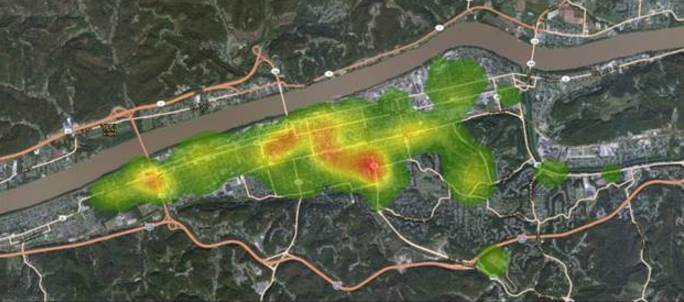
Next, Lemley turned to a much thornier set of data—the number of overdoses in his city.
At first, Route Fifty asked him what the process of gathering that data was like. He just had one word: “long.” And why is it so difficult?
“You have the [Health Insurance Portability and Accountability Act] regulations, the privacy issues. Then, you have the siloes of information,” Lemley said. “9-1-1 . . . has some information, fire has some information, hospitals [have] some more information.” To get it all in one place was a significant challenge.
One factor that contributes to the difficulty is the fact that Lemley wants to be able to track all overdoses, not just those that were fatal. And, in West Virginia, a non-fatal overdose is not a mandatory reportable event.
“If someone goes into the hospital for a survivable gunshot wound, that information has to go to the state somewhere to report it.” The same is not true if you survive an overdose. Law enforcement and emergency medical services are not required to file any paperwork for a person who survives an overdose.
As Lemley put it, there’s often no paper trail for someone who wakes up.
“EMS will revive them, and then they will refuse to go to the hospital.” In that case, EMS will have a record that they made a run for an overdose, but unless you have a relationship with EMS, you’re not getting that information.
Lemley does have a relationship with EMS. And, because he has a relationship with almost every other relevant stakeholder, he believes there are very few non-fatal overdoses that escape his data dragnet.
But, very few places have someone like him to scour for that information. It’s no surprise therefore that the statistics for these types of survived overdoses are vastly undercounted.
Counting the Deaths Isn’t Just Hard in West Virginia
Compiling overdose data has been a major obstacle all over the country.
Nationally, the classification methods being used to count opioid deaths on death certificates may be resulting in substantial undercount of those deaths, according to an academic paper published in 2015 in Public Health Reports, the official journal of the U.S. Public Health Service and the U.S. surgeon general.
When someone dies from an overdose, local coroners or medical examiners determine the cause of death and complete a death certificate. That death is then coded using guidelines called the International Classification of Diseases Tenth Revision, commonly called ICD-10.
This system falls short when it comes to accurately recording opioid deaths. For example, if a coroner happens to have determined which drug was involved in the death—was it heroin? Or fentanyl? Or tramadol?—the appropriate and precise ICD-10 code will be attached to that certificate. If the coroner writes “opioid” alone, that classification will likewise be much less specific.
But, if a coroner or ME does not complete a test to determine the drug that caused the death and simply writes “drug overdose” on the certificate, the death will receive the classification of “other and unspecified drugs.” Because those last deaths might also include people who died from non-opioid drugs, they are not officially counted in the opioid overdose statistics.
Upon examination of this system, a team of researchers found significant numbers of deaths around the country that have been counted as having been caused by “other and unspecified drugs.” In Kansas and Michigan, more drug overdose deaths were attributed to that unspecified category of drugs than were attributed to opioids. “It is possible, even likely,” according to the report, “that a significant proportion of the overdoses due to “other and unspecified drugs” in these states was in fact due to opioid analgesics.”
Not only is this national data likely to be underreported, it’s also slow to be released. In January, the U.S. Centers for Disease Control and Prevention released its figures for 2015, but before that, the lag time on data was two years long.
In a piece on the opioid epidemic by PBS’ Frontline, Tom McLellan, the former deputy director of the Office of National Drug Control Policy compared designing policy around a two-year delay in data to “driving by looking in the rearview mirror.”
Why It’s Worth It
The delay on national-level data is something that gets Lemley fired up—in an interview with Route Fifty, the volume of his voice went up and he started to talk a bit faster.
“When the delay is two years long, that’s worthless to us,” he says. “We get quarterly, sometimes monthly economic data, but when it comes to drug overdoses we have to wait two years. It’s about setting priorities. It’s absolutely insane.”
Lemley channels this passion into uncovering the data for his city. If he had enough time, he says he would update his data every day. But as it is, it’s updated on average once per month.
The search for the data on Huntington’s overdoses may be laborious, but it’s work he knows is worth the effort, particularly in a place like Huntington with big opioid abuse problems, and strained budgets.
“We’re a small city with limited resources, we have to be smarter about where we target enforcement efforts and where we target resources to get people help.”
Now, Lemley isn’t just looking at the number of overdoses, he’s crafting inventive combinations of variables to create data sets that have the power to shape policy.
For example, on a whim he wondered if he would find anything interesting if he cross-checked overdoses in Cabell County, where Huntington is located, by hour of the day. This is what popped up:
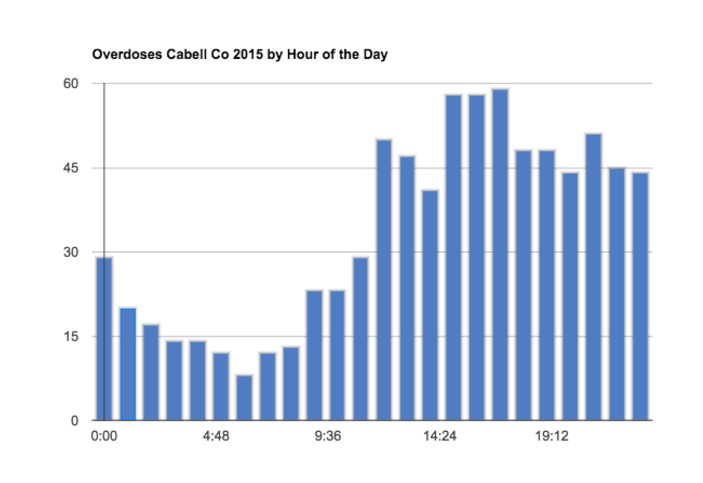
In the chart, there’s a huge spike from 11 a.m. to noon. And that spike continues to 11 p.m. and then drops off at midnight. Lemley says this pattern wasn’t true in the days of crack and cocaine—when hour of the day didn’t seem to make any difference.
The best part of this, for Lemley is that his data is free. “I’ll share it with anybody and everybody,” once it’s been scrubbed of any privacy-compromising data. He shares it with local health care providers so they can plan staffing, he shares it with emergency services so they know what hours of the day to be especially prepared.
Another revelation came when Lemley cross-referenced data gathered at Huntington’s needle exchange with the overdoses in the city. ZIP code data is collected from clients of the syringe program, and by plugging that data into a program built by Esri, the Redlands, California-based geographic information systems software company, he found something shocking. He realized that the majority of the overdoses weren’t coming from the same ZIP codes as the needle exchange clients.
The data revealed a gap in Huntington’s response to the epidemic, and affirmed the need to expand needle exchange services. Lemley acknowledged that whether there are funds for those projects in that region of West Virginia is a different story, and it’s one that Route Fifty has reported on in the past.
Lemley also acknowledged that hindsight for the shift that took place in 2011 is 20/20. But with a sharp eye toward data, he’s moving toward a system that he hopes would allow him to act quickly to fight whatever comes next.
Quinn Libson is Staff Correspondent for Government Executive's Route Fifty and is based in Washington, D.C.

NEXT STORY: Kentucky Gov. Matt Bevin on Medicaid: ‘We Need to Rethink the System’