Connecting state and local government leaders
But the data and the on-the-ground experience of local health officials beg to differ.
WASHINGTON — Republicans in the U.S. Senate are trying out an interesting scapegoating tactic when it comes to the escalation of the nation’s opioid crisis. They are pointing the finger of blame at Medicaid, the federal-state program that provides health care coverage to millions of low-income Americans.
On Wednesday, the Senate Homeland Security and Governmental Affairs Committee, chaired by Wisconsin Republican Ron Johnson, held a hearing with the stated intention of revealing the “unintended consequences” of Medicaid with regard to the nationwide epidemic.
And, a report from Johnson, also released on Wednesday, links Medicaid and expansion of the program under the Affordable Care Act with the increase in overdose deaths.
The gist of that report—and the line of questioning from many of the Republican senators during Wednesday’s hearing—was essentially this: that Medicaid has increased patients’ access to prescription opioid drugs, which are then abused and diverted to the black market, fueling both the rise in addiction and death. This isn’t the first time Johnson and other Republican lawmakers have floated this claim.
In late July 2017, at the height of the GOP push to repeal and replace the Affordable Care Act, Johnson wrote a letter to the Health and Human Services Department’s inspector general alleging a correlation between Medicaid expansion and opioid overdoses. “Because opioids are so available and inexpensive through Medicaid,” Johnson wrote, “it appears that the program has created a perverse incentive for people to use opioids, sell them for large profits, and stay hooked.”
And it isn’t just conservative lawmakers in Congress who are trying out this argument. Louisiana’s Republican attorney general, Jeff Landry, asserted in November that his state’s decision to expand Medicaid had fueled its opioid crisis. “A program that just gives away drugs, without the proper protocols in place, certainly has exacerbated this condition,” Landry said.
The Data Tells a Different Story—in Louisiana, and Across the Nation
In response to Landry’s claim, Esteban Gershanik, the Louisiana Department of Health and Hospitals’ chief information officer told WAFB-TV, the local CBS affiliate in Baton Rouge: “I don't know where the Attorney General got his numbers.”
According to Gershanik, the number of opioid pills being prescribed is actually on the decline in in Louisiana. At the time, the Louisiana Board of Pharmacy Prescription Monitoring Program projected the number of prescriptions per 100 Louisiana citizens in 2017 to be around 109. That’s a decrease from 113 in 2015 and 110 in 2016, the year the state’s Medicaid expansion went into effect.
“Those things that often make you addicted—the amount of opioid pills and the number of opioid pills—has decreased by 25 percent over the past three months,” Gershanik said in November.
Louisiana isn’t the only place where the causal relationship between Medicaid expansion and the opioid crisis appears tenuous, at best. Across the country, the argument that Medicaid expansion catalyzed or worsened the overdose crisis crumbles with an examination of the timeline and evolution of the epidemic.
The Timeline Argument
Conservative pundits and politicians are trying to establish a connection between the ACA’s Medicaid expansion and a rise in overdose deaths related to the opioid crisis.
During Wednesday’s hearing, Sam Adolphsen, a senior fellow at the Foundation for Government Accountability—an organization whose stated mission is to equip policymakers “with principled strategies to replace failed health and welfare programs nationwide”—testified that 13 of the 15 states with the highest age-adjusted rates of opioid overdose deaths are Medicaid expansion states.
“This correlation is deeply concerning. Is the addition of tens of millions of able-bodied adults to Medicaid partly responsible for the opioid crisis?” Adolphsen asked.
While there might be a correlation here, researchers have been unable to show any causation. In August 2017, partly in response to Johnson’s aforementioned letter, Andrew Goodman-Bacon, an assistant professor of economics at Vanderbilt University, and Emma Sandoe, a health policy Ph.D student at Harvard University, took on an analysis of the available evidence that the Medicaid expansion caused the opioid epidemic, and published their findings in Health Affairs. Their conclusion: “there’s little evidence” to support that claim.
Goodman-Bacon and Sandoe found that the claim that expansion of Medicaid caused or exacerbated the opioid epidemic is not credible for three primary reasons:
First, trends in opioid deaths nationally and by Medicaid expansion status predate the ACA. Second, counties with the largest coverage gains actually experienced smaller increases in drug-related mortality than counties with smaller coverage gains. Third, the fact that Medicaid recipients fill more opioid prescriptions than non-recipients largely reflects greater levels of disability and chronic illness in the populations that Medicaid serves. While we do not reject the possibility that public policy has played a role in our current prescription abuse crisis, on balance we find little evidence to support the idea that Medicaid caused or worsened the epidemic.
The timeline argument—that the worsening of the opioid epidemic predates the move by states to expand Medicaid—is perhaps the most persuasive. This chart, for example, shows that the states that would later go on to expand Medicaid were seeing higher rates of drug poisoning mortality years before expansion began in 2014.
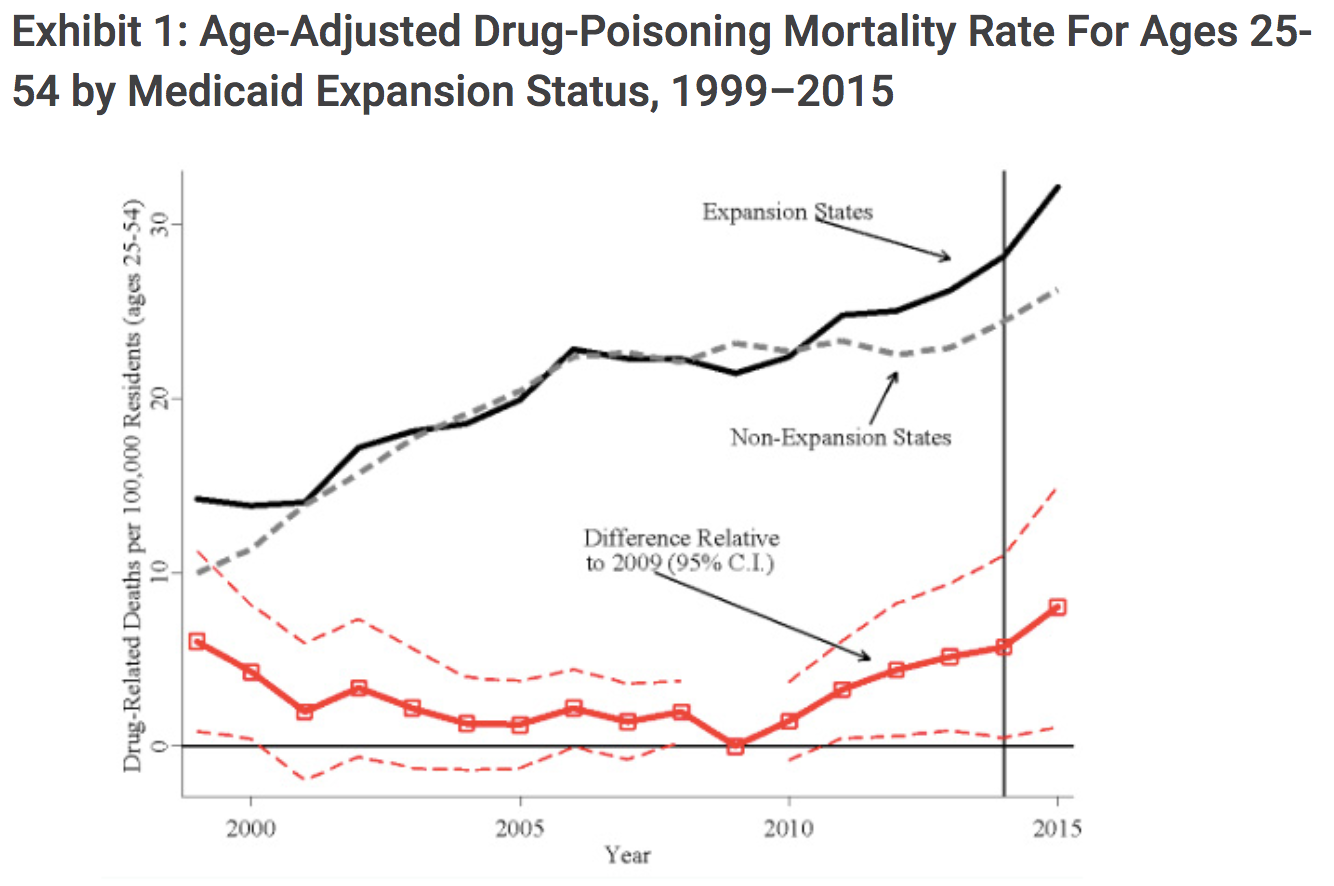
The Trends Argument
The timeline isn’t the only data point that simply doesn’t match up to this GOP claim. The evolution of the epidemic itself has meant that prescription painkillers, like the ones conservative pundits argue were newly available to Medicaid beneficiaries following expansion, are not the driving force behind the recent surge in deaths.
Experts and the data agree: the catalyst behind skyrocketing overdose deaths is not prescription painkillers. Instead, devastatingly deadly synthetic opioids like fentanyl and carfentanil are to blame.
Research has shown that, in fact, the number of opioid painkiller prescriptions being written is on the decline. While prescribing remains alarmingly high in many parts of the nation, since a peak in 2010, the U.S. has seen year-after-year reductions in the writing of these prescriptions. And the results of that decline in prescribing are born out in the latest mortality data.
Age-adjusted drug overdose death rates, by opioid category: United States, 1999–2016
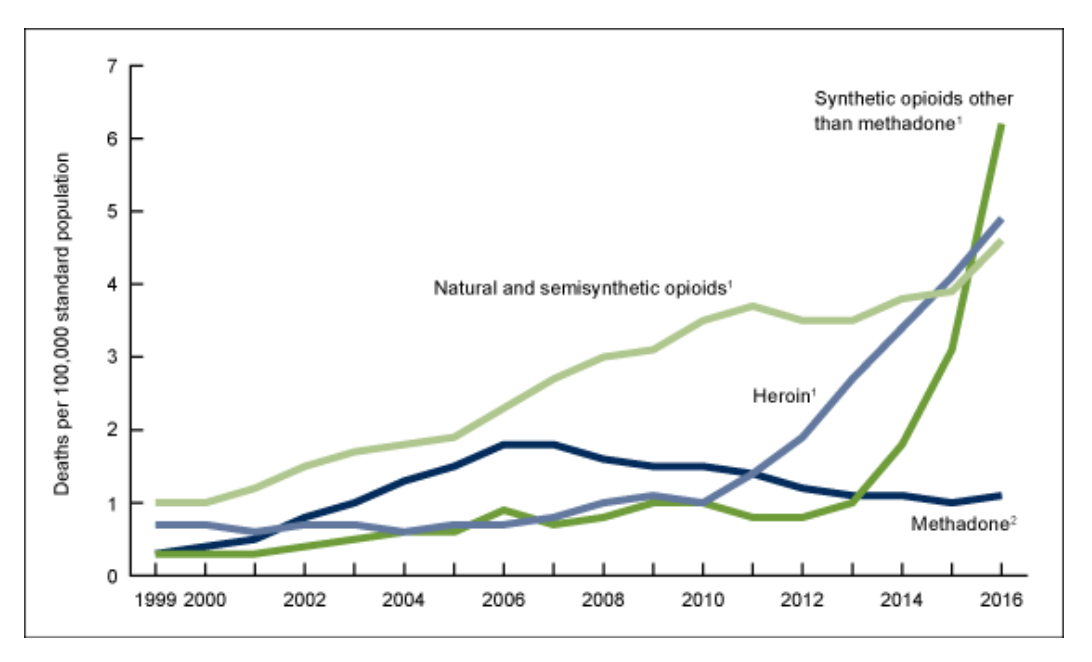
As the chart from the U.S. Centers for Disease Control and Prevention shows above, while deaths related to natural and semisynthetic opioids—a category that includes prescription painkillers—have mostly plateaued, deaths related to synthetics like fentanyl have exponentially increased. In fact, these types of deaths increased so rapidly that the rate of such overdoses doubled in a single year from 3.1 per 100,000 in 2015 to 6.2 in 2016.
If Medicaid expansion, and the resulting access to prescription drugs, were to blame for the spike in overdose deaths, we would be looking at a very different chart, with prescription drugs leading the pack in terms of cause of death.
The View From the Trenches
Health officials and advocates would disagree with the conservative assessment of Medicaid’s role in the crisis for another reason: they have seen what Medicaid expansion has done, and the impact the program has had on connecting those suffering from substance abuse disorders with treatment.
An analysis by the Kaiser Family Foundation found that a growing number of nonelderly adult Americans are having their opioid addiction treatment covered by the federal program—26 percent of were receiving treatment covered by the program in 2005, 10 years later that percentage had doubled:
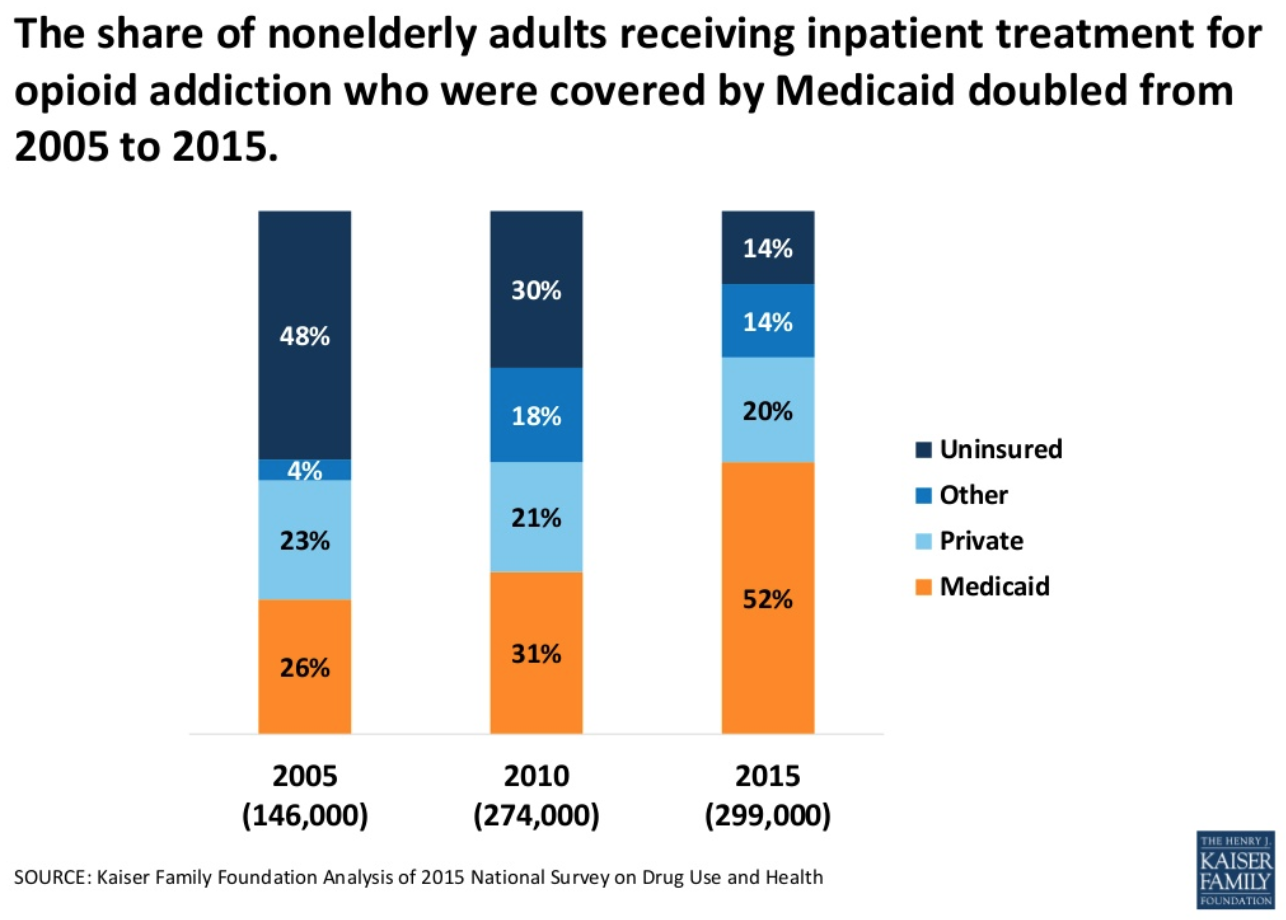
“Medicaid expansion has been, from my perspective in the trenches, the most powerful tool that we have policy-wise to get people into recovery,” Dr. Michael Brumage, the executive director and health officer of the Kanawha-Charleston Health Department in West Virginia, told Route Fifty in a phone interview on Wednesday.
“Expanding access to services has been beneficial to get people who would otherwise be in the shadows of the opioid epidemic into treatment,” Brumage added.
Quinn Libson is a Staff Correspondent for Government Executive’s Route Fifty and is based in Washington, D.C.

NEXT STORY: Hazy Outlook for Congressional Response to Justice Dept.'s Overhauled Marijuana Guidance




